Understanding Pancreatic Cancer: Causes & Symptoms
Explore the causes and symptoms of pancreatic cancer, along with effective naturopathy and yoga treatment options. Learn how these holistic approaches can support cancer care and improve well-being.
DISEASE
12/24/20257 मिनट पढ़ें
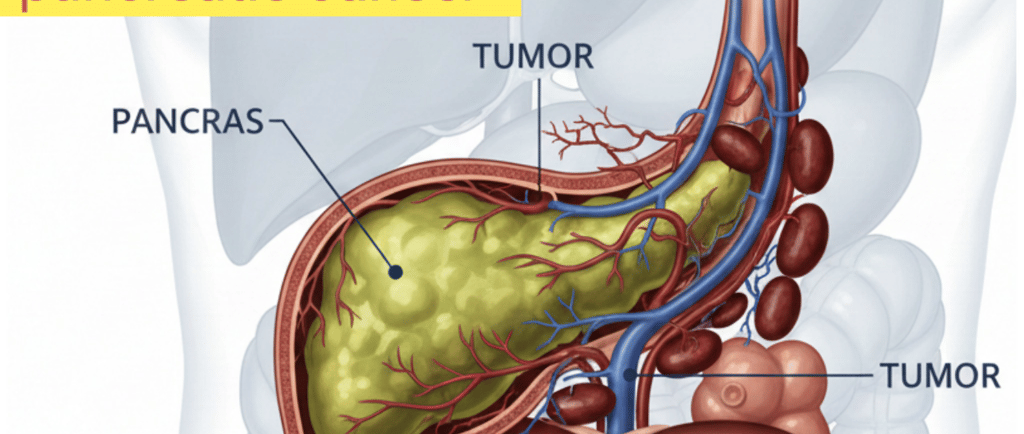
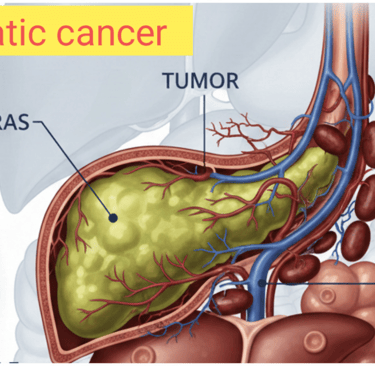
Introduction to Pancreatic Cancer
🙏My dear friend today I told you about pancreatic cancer. Pancreatic cancer is a malignancy that arises from the tissues of the pancreas, an organ located behind the stomach that plays a crucial role in digestion and blood sugar regulation. This type of cancer is particularly insidious due to its aggressive nature and the pancreas's deep anatomical position, which complicates early detection. The two main histological types of pancreatic cancer are exocrine tumors, which constitute the majority, and neuroendocrine tumors, arising from hormone-producing cells.
The development of pancreatic cancer is typically linked to various risk factors, including smoking, obesity, chronic pancreatitis, and family history. The genetic predisposition may influence the risk of developing the disease, as certain inherited mutations have been identified. Early-stage pancreatic cancer often presents no obvious symptoms, which significantly contributes to the late diagnosis faced by many patients. As a result, symptoms such as weight loss, jaundice, and abdominal pain tend to emerge only when the disease has progressed to an advanced stage, making effective treatment more challenging.
Furthermore, the prognosis for pancreatic cancer remains unfavorable when compared to many other cancers, with a five-year survival rate that is notably low. The difficulty in achieving early detection, coupled with the aggressive behavior of the cancer, places a profound emotional and psychological burden on patients and their families. Understanding pancreatic cancer is essential for raising awareness, encouraging preventive measures, and advocating for continued research and improved treatment modalities so that early detection becomes a realistic goal. This awareness is pivotal for enhancing outcomes and ultimately providing hope for those affected.
Causes of Pancreatic Cancer
Pancreatic cancer is a complex disease influenced by a variety of factors that can contribute to its development. Understanding these causes is crucial in the fight against this often fatal condition.
Genetics plays a pivotal role, as individuals with a family history of pancreatic cancer are at an increased risk. Specific inherited genetic mutations, such as those seen in the BRCA2 gene and familial pancreatitis, have been linked to a higher incidence of this cancer. Studies suggest that approximately 10% of pancreatic cancer cases are hereditary, highlighting the importance of genetic counseling for families with a history of the disease.
Lifestyle choices significantly impact the risk profile for pancreatic cancer. Smoking is one of the most established risk factors, with smokers being twice as likely to develop the disease compared to non-smokers. Furthermore, poor dietary habits, including diets high in red and processed meats and low in fruits and vegetables, can also contribute to the risk. Obesity is another critical lifestyle factor, as it is associated with an increased likelihood of both diabetes and pancreatic cancer itself.
Medical conditions, such as diabetes and chronic pancreatitis, are also closely linked to the risk of pancreatic cancer. Research indicates that individuals with long-standing diabetes may see a two-fold increase in their risk. Chronic pancreatitis, typically resulting from long-term alcohol use or hereditary factors, can lead to significant cellular changes in the pancreas that may foster cancer development over time.
In conclusion, there are various interrelated causes of pancreatic cancer, including genetics, lifestyle choices, and pre-existing medical conditions. Awareness of these factors can help guide prevention strategies and early detection approaches in populations at risk.
Common Symptoms of Pancreatic Cancer
Pancreatic cancer is often referred to as a "silent" disease because it frequently exhibits subtle symptoms that can be easily overlooked, particularly in its early stages. Understanding these common symptoms is crucial for timely diagnosis and intervention.
One of the hallmark symptoms of pancreatic cancer is jaundice, which manifests as a yellowing of the skin and eyes. This occurs when the cancer obstructs the bile duct, leading to a buildup of bilirubin in the bloodstream. Jaundice can also be accompanied by itchiness and dark urine, signaling a potential issue that requires prompt medical evaluation.
Abdominal pain is another significant symptom associated with pancreatic cancer. Individuals may experience discomfort or pain in the upper abdomen, which might radiate to the back. This pain can be constant or intermittent, often described as a dull ache or an intense pain that disrupts the patient’s daily activities.
Weight loss is frequently observed in patients with pancreatic cancer, even in the absence of a deliberate effort to lose weight. This unintentional weight loss may be due to the cancer's impact on metabolism and digestion. Patients can also experience changes in appetite, leading to a reduced intake of food, which exacerbates the weight loss issue.
Other associated symptoms may include changes in bowel habits, such as the presence of greasy or oily stools, which indicates malabsorption of nutrients, and the development of diabetes, which can arise from the pancreas's inability to produce adequate insulin. Overall, recognizing these common symptoms of pancreatic cancer is essential for early detection and improving the chances of successful treatment.
Diagnosis of Pancreatic Cancer
The diagnosis of pancreatic cancer typically involves a series of procedures and tests designed to identify the presence of cancerous cells in the pancreas. One of the first steps in this process is a comprehensive evaluation of the patient’s medical history and symptoms. Physicians will often conduct imaging tests such as a computed tomography (CT) scan or magnetic resonance imaging (MRI) to visualize the pancreas and check for abnormalities. These imaging modalities play a crucial role in detecting tumors, assessing their size, and determining whether they have spread to adjacent organs.
Blood tests are also integral to the diagnostic process. Healthcare providers may monitor the levels of specific tumor markers, particularly the carbohydrate antigen 19-9 (CA 19-9), which can be elevated in individuals with pancreatic cancer. However, it is important to note that elevated CA 19-9 levels are not exclusively indicative of cancer, as they can also be caused by other conditions affecting the pancreas. Therefore, blood tests are usually conducted in conjunction with imaging to confirm any findings.
If imaging tests suggest the presence of pancreatic cancer, a biopsy is often performed to obtain a sample of tissue for microscopic examination. Biopsies can be done using various methods, including endoscopic ultrasound-guided fine-needle aspiration or percutaneous biopsy techniques. This definitive test is critical, as it can confirm the diagnosis and provide information about the type and grade of cancer, allowing for more tailored treatment options.
Early detection of pancreatic cancer presents significant challenges due to the absence of specific symptoms in the initial stages of the disease. This often results in a late diagnosis, limiting treatment options and impacting survival rates. Increased awareness and ongoing research into more effective screening methods remain essential in the fight against this aggressive cancer.
Conventional Treatment Options for Pancreatic Cancer
Pancreatic cancer is often treated with a combination of conventional methods, each aimed at addressing the malignancy's unique challenges. The primary treatment options include surgery, chemotherapy, and radiation therapy, each serving distinct purposes in the management of the disease.
Surgery is commonly considered when the cancer is diagnosed at an early stage and is localized to the pancreas. The most common surgical procedure is the Whipple procedure, or pancreaticoduodenectomy, which involves removing the head of the pancreas, the duodenum, and other surrounding tissues. However, surgery is not suitable for all patients, especially if the cancer has metastasized or is located in a region that makes surgical removal difficult.
Chemotherapy plays a crucial role in the treatment of pancreatic cancer, particularly in advanced stages. It involves the use of drugs to kill cancer cells or inhibit their growth. Common chemotherapeutic agents include gemcitabine and FOLFIRINOX. While chemotherapy can contribute to extending life and managing symptoms, it is accompanied by potential side effects, including nausea, fatigue, and increased susceptibility to infections, which can significantly affect a patient's quality of life.
Radiation therapy is often used in conjunction with chemotherapy, either as a neoadjuvant treatment to shrink tumors before surgery or as palliative care to alleviate pain and manage symptoms in advanced cases. This method utilizes high-energy rays to destroy cancer cells; however, patients may experience side effects such as skin irritation and fatigue.
Each of these conventional treatment options presents challenges and potential complications, emphasizing the need for personalized care tailored to the patient’s specific condition and preferences. The side effects associated with these therapies can be significant, often requiring additional supportive measures to help patients cope with their impact.
Naturopathy and Yoga as Treatments
Naturopathy and yoga offer complementary approaches to managing pancreatic cancer, providing patients with holistic care that may enhance conventional treatments. These disciplines emphasize the body’s innate ability to heal, focusing on prevention, nutrition, and lifestyle modifications. This integrative strategy can support not only physical healing but also emotional well-being during challenging times.
In naturopathy, a variety of practices are employed, including dietary recommendations, herbal supplements, and lifestyle changes tailored to the individual's needs. Nutrition plays a pivotal role in managing pancreatic cancer, with an emphasis on a plant-based diet rich in fruits, vegetables, and whole grains. Foods high in antioxidants, such as berries and leafy greens, may help combat oxidative stress and support the immune system. Additionally, certain herbal remedies like turmeric, which contains curcumin, have shown promise in research for their anti-inflammatory and anti-cancer properties.
Alongside dietary practices, naturopaths may suggest detoxification methods to aid in the elimination of toxins, as well as stress management techniques, which are essential for overall health. Practices such as meditation and mindfulness may promote relaxation and potentially enhance the body’s healing capacity.
Yoga complements these naturopathic principles by encouraging physical activity that is gentle yet effective. Specific yoga poses, such as the Cat-Cow Stretch, Child’s Pose, and Legs-Up-the-Wall Pose, can improve flexibility, reduce stress, and enhance circulation. These poses are designed to relieve tension and promote a sense of calm, which can be especially beneficial for patients undergoing traditional treatments.
Incorporating these holistic strategies into a patient's care plan can provide additional support in managing symptoms, enhancing quality of life, and fostering emotional resilience. By integrating naturopathy and yoga alongside conventional therapies, patients may find a more balanced approach to navigating the complexities of pancreatic cancer treatment.
Conclusion and Encouragement for Patients
In the ongoing fight against pancreatic cancer, fostering awareness and understanding plays a crucial role. Recognizing the symptoms early can significantly impact treatment outcomes, prompting timely medical interventions. Patients and their families should remain vigilant about potential warning signs, ensuring that they consult healthcare professionals without hesitation.
It is essential to adopt a comprehensive treatment plan that encompasses not only conventional medical approaches but also holistic therapies. Integrating naturopathy and yoga into the care routines of pancreatic cancer patients can yield remarkable benefits. Naturopathy focuses on enhancing the body’s natural healing abilities through natural remedies and lifestyle changes, which can aid in alleviating symptoms and improving overall well-being.
Yoga, on the other hand, facilitates physical and emotional balance, helping patients cope with the stress and anxiety that often accompany a cancer diagnosis. Incorporating yoga poses, breathing exercises, and mindfulness practices can promote relaxation and enhance the quality of life for patients and their caregivers alike.
For those affected by pancreatic cancer, it is important to remain hopeful and resilient. Surrounding oneself with a supportive network of family, friends, and healthcare providers can foster a more encouraging environment. Remember that exploring different treatment modalities, including naturopathy and yoga, can provide a sense of empowerment in managing health and wellness.
By staying informed and taking proactive steps, patients can navigate this challenging journey with greater confidence. A commitment to both traditional and complementary therapies can pave the way for improved outcomes and a brighter outlook for those impacted by pancreatic cancer.
Contact
Reach us to book your wellness session
Email - rajnaturcure@gmail.com
© 2025. All rights reserved.
